Global awareness of HAE can save lives
The purpose of the awareness day is to spread the word about Hereditary Angioedema (HAE), so patients can receive an accurate diagnosis and appropriate medical care.

HAE Day is globally recognised every year on 16 May to spread awareness and rally support worldwide for the rare life-threatening condition known as Hereditary Angioedema.
The purpose of HAE Day is to educate people worldwide about this hereditary illness and to put a stop to the fear they live in and the wait for their next attack
People no longer have to wait an average of 13 years for an accurate diagnosis and the correct treatment that allows them to lead a healthy life.
According to the South African Hereditary Angioedema Association there are just under 100 patients with a confirmed diagnosis of HAE in South Africa. HAE is estimated to have a prevalence between 1:50 000 and 1:150 000 worldwide.
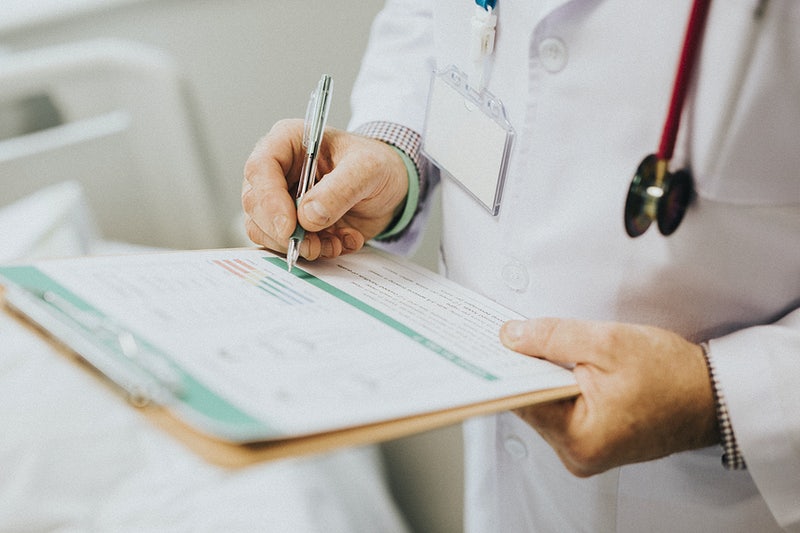
What is Hereditary Angioedema (HAE)?
According to the Executive Vice President and Chief Operating Officer of HAE International, the international patient organisation leading the day, Henrik Balle Boysen, HAE is a rare genetic disorder that causes swelling to various parts of the body, and can be fatal when the swelling affects the throat due to the risk of suffocation.
Global awareness initiatives such as the Hae Day are necessary to help patients receive a faster diagnosis and care to manage the disease, Balle Boysen explains.
Since HAE is a hereditary disorder, it is important to have family members tested. To help patients in this process, two documents were developed for patients and one for physicians, he added.
Symptoms of HAE
The main symptom of HAE is the swelling of the skin, which doctors refer to as ‘edema’, occurring mainly in the face (e.g. lips, eyelids), although the extremities and genitals are often affected.
Swelling of the internal organs, specifically the mucous membranes of the larynx, nose or tongue, is potentially life-threatening as it can cause death by suffocation.
More than 50% HAE patients will experience at least one attack of this type in their lifetime.
According to Balle Boysen, patients are frequently misdiagnosed because HAE symptoms often resemble those of more common conditions.
“Through the 2020 Hae Day, we hope to spread the word about HAE, so patients can receive an accurate diagnosis and appropriate medical care.”
He says they are excited by the level of participation from HAE national organisations across the globe and hope that the awareness day will make a real difference to lives of HAE patients in future.

What is HAE International?
According to HAE International, the global non-profit organisation dedicated to raise awareness for patients who have HAE defect in their genes that controls a blood protein called C1-inhibitor.
The disease is sometimes referred to as a C1-inhibitor deficiency and is considered the primary immunodeficiency of complement proteins. The HAE International network presently consists of 84 national HAE patient organisations spread across the globe.
Says Balle Boysen: “HAE International was established to promote cooperation, coordination and information-sharing between HAE specialists and national HAE patient associations to help facilitate the availability of effective diagnosis and management of C1-inhibitor deficiencies throughout the world.
Our purpose is to join the efforts and experience of the global HAE community to achieve optimal standards of care and treatment for all those patients affected by C1-inhibitor deficiencies”.
HAE places extraordinary strain on those affected by it and can cause restrictions on their daily lives. Left untreated, patients who suffer from HAE can lose up to 150 working days per annum and possibly even more.
There is currently no cure for the disease, however, treatment options are available in an attempt to prevent attacks and to treat attacks when they do occur.

Frequently asked questions about HAE
Q: What is Hereditary Angioedema (HAE)?
A: Hereditary Angioedema (HAE) is a rare genetic disorder characterized by episodes of swelling (edema attacks) in different areas of the skin or the internal organs. In particular, it occurs in the upper respiratory tract and intestine.1,2 Episodes affecting the larynx or tongue are particularly dangerous and can cause death by suffocation if untreated.2,6-8
Q: How many people are affected by HAE?
A: Exact figures regarding the incidence of HAE are not available. It is estimated that about 1 in 10,000 to 1 in 50,000 people are affected worldwide.1,9
Q: When do the symptoms of HAE first occur?
A: Most patients experience their first attack during childhood or adolescence, and then continue to suffer from subsequent attacks throughout the duration of their lives.2
Q: How do the symptoms of HAE manifest themselves?
A: An episode of HAE involves an acute swelling of the skin or mucous membranes, primarily affecting the limbs, face and neck as well as the buttocks and genitalia. Although this swelling of the skin is almost never associated with itching, it causes a feeling of tension, the severity of which ranges from unpleasant to painful. The facial swelling can be disfiguring. Swelling can also occur in the wall of the intestine. This swelling is associated with colicky pain and can cause diarrhoea, vomiting and circulatory disorders. In extreme cases, even intestinal paralysis and intestinal obstruction are possible.1,2,5,10 The most feared complication of HAE is swelling in the larynx (laryngeal edema) or upper respiratory tract, which can cause death by suffocation if left untreated.2,6-8
Q: How often do episodes of HAE occur?
A: The frequency, duration and severity of attacks vary considerably. Approximately 22 per cent of patients report a frequency of greater than one attack per month; 40 per cent of patients experience on average 6 to 11 attacks per year, and the remaining 22 per cent are infrequently symptomatic.1
Q: How long does an episode of HAE last?
A: In most cases, the symptoms of HAE are transient, progressing over 12 to 36 hours, and then subsiding gradually over the next two to five days. However, some patients may experience attacks that last over a week.1,5 Although HAE episodes are self-limiting, the unpredictable occurrence of attacks places considerable strain on patients, often restricting their ability to lead normal lives. Untreated, patients with HAE lose up to 100 to 150 workdays per year and have morbidity approaching 50 per cent.11
Q: Why can certain episodes of HAE be life-threatening?
A: If an episode of HAE involves laryngeal attacks this may lead to airway obstruction and have the potential to cause death by asphyxiation.2,6-8 Amongst HAE patients suffering from edema of the larynx, the estimated mortality rate of untreated attacks is as high as 40 per cent if the attack is not treated adequately.10 If the mucous membranes in the larynx start to swell, immediate medical treatment is required. It may be necessary to intubate the patient or make an emergency incision in the windpipe (tracheostomy) if appropriate treatment is not available.
Q: What causes HAE?
A: HAE is caused by a genetic defect on chromosome 11, which leads to a deficiency of the protein C1-esterase inhibitor (C1-INH). This protein is part of a system known as the complement system, which is involved in the complex interaction leading to immune and inflammatory reactions in the body. Among other things, C1-INH controls the release of the tissue hormone bradykinin. If either C1-INH concentration or activity is decreased, bradykinin concentrations may increase and an episode of swelling can occur. There are two types of HAE. Type I is the most common (approximately 85 per cent of cases) and involves a C1-INH deficiency resulting from insufficient production of the enzyme. Type II affects approximately 15 per cent of patients and involves normal or even elevated C1-INH concentrations but reduced C1-INH activity (function). Recently, a rare third form of the disease has been discovered. Unlike the other two subtypes of HAE, this subtype is not associated with a C1-INH deficiency. It affects mostly women and is reported to be associated with a mutation of factor XII.12,13,14
Q: What triggers an episode of HAE?
A: Episodes of HAE often occur without an obvious trigger. However, in some cases, a cause can be identified. For instance, infections, minor injuries and mechanical stimuli such as pressure can induce an attack.
Dental procedures or surgery to remove the tonsils are particularly critical, as they can cause swelling in the larynx. Emotional and mental stress can also trigger an attack.
Hormonal factors are another known cause of HAE attacks. For example, the frequency of episodes can be higher in women taking products containing estrogen (“the pill”), products for menopausal complaints, or who have their menstruation. A class of blood pressure-lowering drugs known as ACE (angiotensin-converting enzyme) inhibitors are contraindicated in HAE patients as they have also been shown to trigger HAE attacks in some patients. HAE patients should, therefore, avoid taking this type of medication.
Q: What does the fact that HAE is a hereditary disease mean?
A: The defect on chromosome 11 that is responsible for HAE is equally common in men and women and can be passed on by both sexes. As HAE is an autosomal dominant hereditary disease, there is a 50 per cent risk of a child inheriting the disease from the affected parent. Male and female offspring are at equal risk of inheriting HAE.
Q: How can you tell if the larynx is starting to swell?
A: The larynx can swell both spontaneously and after an injury to the oral mucosa, e.g. during dental treatment. The first signs will be difficulty swallowing, voice changes and hoarseness. Increasing swelling in the larynx then leads to breathlessness, which can cause suffocation in extreme cases. If a patient experiences these symptoms, he or she should seek medical help immediately.
Q: How is HAE diagnosed?
A: If the patient has recurrent episodes of edema affecting the limbs, face, neck or buttocks and lasting several hours to days, HAE should be considered as a diagnosis. HAE can also be the cause of recurrent colicky pain in the abdominal cavity. If a family history is already known to include cases of HAE, it is very reasonable to suspect HAE the first time it occurs in another family member. Failure to respond to drugs administered for allergic reactions, such as antihistamines, corticosteroids and adrenaline, is also used to distinguish HAE from allergic edema. However, the diagnosis of HAE is confirmed by special blood tests in which the concentration and activity of C1-INH and the concentrations of other proteins in the complement system are measured. The concentration and/or activity of C1-INH are reduced in patients with HAE.
Q: What does HAE mean for a pregnancy and vice versa?
A: In principle, women with HAE can have children. HAE does not impair fertility. However, women who are being treated with androgens should stop taking them, as this treatment can impair female fertility. Episodes of HAE can increase or decrease during pregnancy, as can the severity of the edema. Your doctor will follow you closely during this time and discuss appropriate treatment with you.
Q: Why does it often take years to diagnose HAE?
A: HAE is a rare and relatively unknown disease. In addition, the symptoms of an episode of HAE are similar to those of much more common diseases, e.g. an allergy or appendicitis. This makes it difficult to diagnose HAE correctly. HAE can also be confused with other forms of angioedema, e.g. allergic angioedema. However, the drugs used to treat this form of angioedema, such as cortisone and antihistamines, have no effect on the symptoms of HAE. Diagnosing HAE is particularly difficult if the patient suffers predominantly from gastrointestinal attacks. If HAE is suspected, the diagnosis can be confirmed quickly by a blood test.
Q: What treatment options for HAE are available?
A: There are three established treatment options for HAE: acute treatment, long-term prophylaxis and short-term prophylaxis.
Q: When is the acute treatment of HAE necessary?
A: The aim of acute treatment is to stop the progression of the edema and to resolve the symptoms. This applies particularly to episodes in the larynx, which can cause death if left untreated.
Q: What options are available for acute treatment?
A: The recommended options for acute treatment vary from country to country due to the fact that drugs for specific treatment are not licensed in all countries. In these cases, acute treatment may be limited to more unspecific drugs such as tranexamic acid or even just painkillers. In countries where it is available, Icatibant or C1-INH concentrate can be used for the treatment of acute attacks. Icatibant must be administered by subcutaneous injection by a healthcare professional, C1-INH concentrate must be administered intravenously.
Q: What is the aim of long-term prophylaxis?
A: Long-term prophylaxis is indicated in patients whose quality of life is clearly reduced by the disease. These are usually patients in whom episodes occur more than once a month or who are at high risk of developing laryngeal edema. The aim is to reduce the frequency and/or the severity of HAE attacks.
Q: When is short-term prophylaxis necessary?
A: Short-term prophylaxis is usually performed before surgical procedures or dental treatment. In countries in which C1-INH concentrate is available, it is administered 60 to 90 minutes before the procedure as an intravenous infusion. In all other countries in Europe high-dose treatment with androgens is administered for 5-7 days beforehand.
Sources
- Agostoni A, Aygoren-Pursun E, Binkley KE, et al. Hereditary and acquired angioedema: problems and progress: proceedings of the third C1 esterase inhibitor deficiency workshop and beyond. J Allergy Clin Immunol 2004;114(3 Suppl):S51-131.
- Bork K, Meng G, Staubach P, Hardt J. Hereditary angioedema: new findings concerning symptoms, affected organs, and course. Am J Med 2006;119(3):267-74.
- Jesic R, Culafic D, Bonaci-Nikolic B. Hereditary angioedema presenting with recurrent ascites. Dig Dis Sci 2005;50(1):24-6.
- Branco-Ferreira M, Pedro E, Barbosa MA, Carlos AG. Ascites in hereditary angioedema. Allergy 1998;53(5):543-5.
- Bork K, Staubach P, Eckardt AJ, Hardt J. Symptoms, course, and complications of abdominal attacks in hereditary angioedema due to C1 inhibitor deficiency. Am J Gastroenterol 2006;101(3):619-27.
- Bork K, Barnstedt SE. Laryngeal edema and death from asphyxiation after tooth extraction in four patients with hereditary angioedema. J Am Dent Assoc 2003;134(8):1088-94.
- Bork K, Hardt J, Schicketanz KH, Ressel N. Clinical studies of sudden upper airway obstruction in patients with hereditary angioedema due to C1 esterase inhibitor deficiency. Arch Intern Med 2003;163(10):1229-35.
- Bork K, Siedlecki K, Bosch S, Schopf RE, Kreuz W. Asphyxiation by laryngeal edema in patients with hereditary angioedema. Mayo Clinic Proc 2000;75(4):349-54.
- Bowen T, Cicardi M, Bork K, et al. Hereditary Angiodema: a current state-of-the-art review, VII: Canadian Hungarian 2007 International Consensus Algorithm for the Diagnosis, Therapy, and Management of Hereditary Angioedema. Ann Allergy Asthma Immunol 2008;100(1 Suppl 2):S30-40.
- Data on file.
- Bracho FA. Hereditary angioedema. Curr Op Hematol 2005;12(6):493-8.
- Dray A. Kinins and their receptors in hyperalgesia. Can J Physiol Pharmacol 1997;75(6):704-12.
- Bas M, Adams V, Suvorava T, Niehues T, Hoffmann TK, Kojda G. Nonallergic angioedema: role of bradykinin. Allergy 2007;62(8):842-56.
- Kaplan AP, Joseph K, Silverberg M. Pathways for bradykinin formation and inflammatory disease. J Allergy Clin Immunol 2002;109(2):195-209. pathophysiology of angioedema. Int Immunopharmacol 2003;3(3):311-7.
Notice: Coronavirus reporting at Caxton Local Media aims to combat fake news
Dear reader,
As your local news provider, we have the duty of keeping you factually informed on Covid-19 developments. As you may have noticed, mis- and disinformation (also known as “fake news”) is circulating online. Caxton Local Media is determined to filter through the masses of information doing the rounds and to separate truth from untruth in order to keep you adequately informed. Local newsrooms follow a strict pre-publication fact-checking protocol. A national task team has been established to assist in bringing you credible news reports on Covid-19.
Readers with any comments or queries may contact National Group Editor Irma Green (irma@caxton.co.za) or Legal Adviser Helene Eloff (helene@caxton.co.za).
Read original story on lowvelder.co.za
