Sara Dalby never imagined she would one day operate on patients when she started studying nursing.

But with Britain facing a shortage of doctors accentuated by Brexit, Dalby and fellow highly-skilled nurses have led the way in a reform already developed in North America.
“I didn’t know these roles existed when I started; I didn’t know I was going to go into (the operating) theatre either,” the 35-year-old based at Aintree University Hospital in the northern city of Liverpool told AFP.
Advanced Nurse Practitioners (ANPs) like Dalby are considered increasingly important in Britain, where unprecedented pressure on the National Health Service (NHS) has seen a shortage of both doctors and funding.
The changing role of nurses “can potentially contribute towards that solution. I don’t think they’re the solution but they could potentially be used to help in some areas,” Dalby said.
ANPs are also helping meet the changing needs of Britain’s ageing population at a time when the prospect of Brexit is prompting European doctors working in the NHS to have doubts about staying.
The NHS in England last year already had a shortage of 6,500 family doctors and that shortfall is expected to rise to 12,100 by 2020, according to a recent estimate by Imperial College London.
A survey of some 2,000 European doctors in the NHS by the General Medical Council earlier this year found that 60 percent were considering leaving Britain.
– ‘Real autonomy’ –
Dalby started out as a nurse in 2003 and is now qualified to conduct facial skin cancer excisions and carpal tunnel surgery without a surgeon present.
ANPs can make independent diagnoses and care plans, as well as engage in more complex areas like surgery.
While they operate under varying levels of supervision, they have significant independence.
They typically earn more than nurses not in advanced practice but less than doctors and consultants.
ANPs began to proliferate in Britain following a 2006 change in the law.
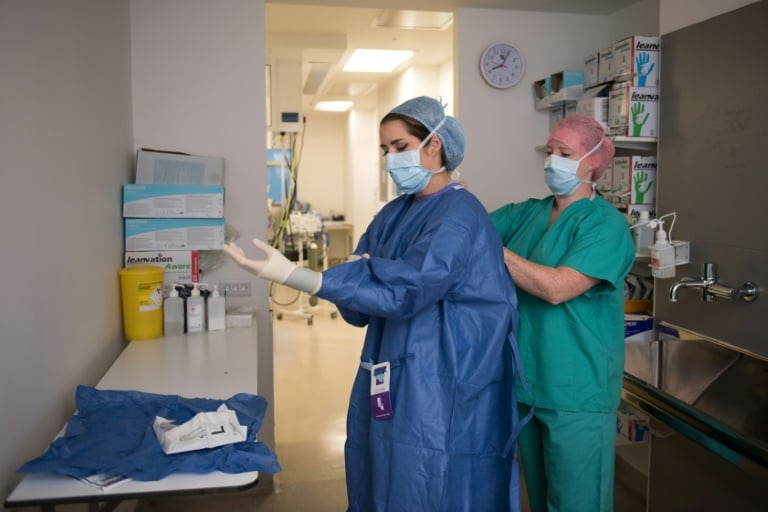
There are thousands of ANPs working in Britain
No single organisation tracks their number, but Wendy Preston, head of nursing practice at the Royal College of Nursing (RCN), estimates thousands now operate in an array of fields.
“That change to legislation really opened out the ability for the nurse to be an independent practitioner and have real autonomy,” Preston said.
Danny Mortimer, head of NHS Employers, a not-for-profit organisation, said the roles offer “a new opportunity for progression and career development for those who do not wish to move into management.”
“And (they) have been shown to provide consistently high levels of patient care and outcomes,” he added.
The trend has not received universal acclaim.
Some healthcare leaders expressing concern at the lack of regulation within the sector, citing cases of nurses unqualified for advanced roles still fulfilling such duties.
But as Dalby’s case shows, becoming an ANP is far from easy. She embodies the time, persistence and patience required to reach this level, and the opportunities that can then open up.
Dalby acquired a Masters in advanced nursing practice and Masters-level qualifications in surgical care practice, all while working full time to build up clinical experience.
She now works in four specialities, as well as lecturing at Edge Hill University, co-authoring a textbook and working more administratively at the RCN and Royal College of Surgeons (RCS).
Ian Eardley, senior vice president of the RCS, said ANPs like Dalby are often “the glue that holds surgical teams together.”





